View sample cancer research paper on bladder cancer. Browse other research paper examples for more inspiration. If you need a thorough research paper written according to all the academic standards, you can always turn to our experienced writers for help. This is how your paper can get an A! Feel free to contact our writing service for professional assistance. We offer high-quality assignments for reasonable rates.
Descriptive Epidemiology
Bladder cancer is three to four times more frequent in men than in women in most populations (Parkin et al., 1999). This is mainly due to men’s higher exposure to the two main recognized risk factors for bladder cancer: tobacco smoking and aromatic amines.
Academic Writing, Editing, Proofreading, And Problem Solving Services
Get 10% OFF with 24START discount code
Transitional-cell carcinoma (TCC) is the most common histological type of bladder cancer, although the distribution of histologies varies in different populations. TCC accounts for over 95% of bladder cancers in white populations, for about 85% in black American populations, and for a lower proportion in Middle East populations, among whom squamous-cell type is frequent. Tobacco smoking and occupational exposures are the main determinants for both TCC and non-TCC bladder tumors.
As concerns the subsite of origin within the bladder, in a large U.S. investigation about 43% of bladder cancers occurred at an unspecified subsite, and 13% arose in more than one subsite. Of bladder cancers occurring in a single subsite, most occurred on one of the bladder walls (40% on lateral walls, 11% on the posterior wall, and 3% on the anterior wall). Less common subsites included the ureteric orifice (17%), followed by the trigone (13%), dome (9%), and neck (7%).
Substantial variability exists in the rates recorded in various cancer registries, partly reflecting different diagnostic criteria, since the distinction between benign and malignant tumors is not straightforward. Thus, bladder cancer incidence rates and trends are difficult to interpret. These cautions notwithstanding, the highest incidence rates are recorded in Europe and North America, although Northern Africa and Western Asia are high-risk areas, too (Parkin et al., 1999).
Mortality rates are more informative. Data on mortality are available from the World Health Organization in a uniform and standardized format for most of Europe, and for selected extra-European countries, including the United States and Japan. In most European countries, male bladder cancer mortality rates (age-standardized, world standard population) in early 2000 ranged between 5 and 8/100 000, whereas rates for women varied between 1 and 2/100 000, the highest rates being observed in Denmark (2.6) and the UK (1.8). In the United States, bladder cancer mortality rates were 3.7/100 000 in men and 1.1 in women; corresponding values in Japan were 2.5/100 000 in men and 0.7/100 000 in women. Bosetti et al. (2005) provided mortality data for some countries of Central and South America, where bladder cancer mortality rates in the year 2000 varied between 1.0 (in Ecuador) and 4.6 (in Argentina) in men and between 0.6 (in Ecuador and Mexico) and 1.1 (in Chile, Cuba, and Puerto Rico) in women. These marked differences across South American countries probably reflect different smoking habits and patterns, such as use of black tobacco, which is strongly associated with bladder cancer, in Argentina and Cuba.
With reference to trends over time, male rates (Figure 1a) in the European Union (EU) were 6.7/ 100 000 in 1970–74, peaked at 7.4 in 1985–89, and declined thereafter to 6.1/100 000 in 2000–01. Important differences, however, existed in different regions, as mortality rates were still increasing in many countries of Eastern Europe, including Bulgaria, Poland, and Romania. In the United States, male bladder cancer mortality rates rose until the mid- 1970s to a value of 5.1/100 000, and then started to decline (Bosetti et al., 2005), that is, about 10–15 years prior to the EU, whereas in Japan the rates were stable around a value of 2.4/100 000 between 1970 and 2001. For women (Figure 1b), mortality rates from bladder cancer in the EU were 1.5/100 000 in 1970–74, 1.6 in 1975–79, and declined thereafter to 1.3 in 2000–01. In the United States, female rates increased to 1.5/100 000 during the 1970s and then declined, as observed in men. In Japan, female mortality rates constantly tended to decrease between 1970 and 1995, and then leveled off (from 0.9/100 000 in 1970–74 to 0.7 in 2000–01). Data on mortality trends from Central and South America are less clear, with some countries showing declining rates from the 1970s (e.g., Argentina and Venezuela), others with fairly constant levels, and a few others that showed a steep increase in male rates after 1995 (e.g., Cuba, Costa Rica, Puerto Rico), possibly reflecting the patterns of tobacco smoking for subsequent generations of American men (Bosetti et al., 2005).
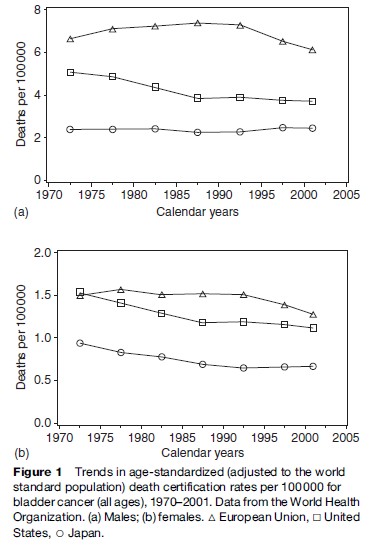
Although problems of case ascertainment and death certification may have affected bladder cancer mortality certification, the trends observed in Europe and other developed areas of the world are probably real, and well reflect the pattern of exposure to tobacco smoking – and to a lesser extent occupational carcinogens – of subsequent generations of men. The pattern of mortality from bladder cancer is similar to that of lung cancer, with downward trends over the last decade in several southern and northern European countries – 10–15 years later than in the United States – and still appreciably upward in some Eastern European countries, where tobacco control is less implemented.
Symptoms And Diagnosis
The main signs of bladder cancer are hematuria (often frank and painless), frequent and/or urgent urination, and painful urination. Although these symptoms are frequently related to other urinary tract conditions, such as cystitis and bladder stones, their medical evaluation is critical, particularly for gross hematuria.
Classic methods to diagnose bladder neoplasms include cystoscopy (passing a tube through the urethra to examine the inner lining of the bladder), urine culture and cytology, followed by transurethral biopsy/resection. Histological analyses of small samples of tissue provide the diagnosis. Although many urinary markers showed promising results as diagnostic or screening tools for bladder cancer, none has yet been proven sufficient for diagnosing or excluding bladder neoplasms.
Screening practices are currently not recommended for bladder cancer, even in high-risk groups (e.g., occupationally exposed subjects), due to high proportions of false-positive results. Clinical studies of screening have failed to demonstrate a beneficial effect on outcome or mortality (Silverman et al., 2006).
Risk Factors
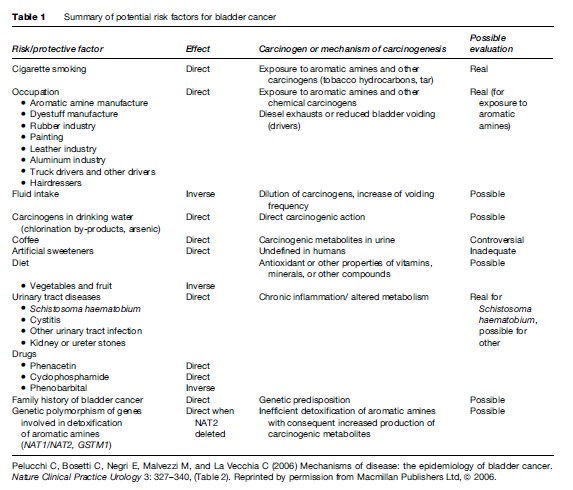
Several epidemiological studies investigated in different populations the role of potential risk factors in bladder carcinogenesis, and a few etiological agents are now established. Known or potential etiological factors for bladder cancer are summarized in Table 1, and are discussed in the following sections.
Tobacco
Cigarette smoking is the main recognized cause of bladder cancer in both developed and developing countries for which data are available. The risk in smokers is two to four times that of nonsmokers, and increases with number of cigarettes per day and duration of smoking. Risk is up to fivefold higher in heavy and in long-term smokers as compared to never-smokers. Smokers of unfiltered, high-tar, or black (air-cured) tobacco cigarettes (i.e., those with higher levels of aromatic amines) are at higher risk than smokers of filtered, low-tar, or blond (flue-cured) tobacco ones. It has been suggested that bladder cancer risk may be higher in women than in men who smoke comparable numbers of cigarettes, but recent investigations and combined reanalysis of earlier studies did not support this hypothesis.
Cessation of smoking led to a 30–60% decrease in risk as compared to current smokers. Though the risk declines with increasing time since quitting, it does not approach that of never-smokers even after 25 or more years since cessation of the habit.
There is some evidence that pipe and cigar smoking are also associated with bladder cancer risk, though not all findings were consistent, whereas there is no evidence from epidemiological data that link smokeless tobacco consumption (i.e., chewing tobacco and snuff ) to bladder neoplasms.
To date, only a small number of studies have provided information on the relation between exposure to environmental tobacco smoke and bladder carcinogenesis, finding inconsistent results.
Occupation
Control of occupational carcinogens has been an important contributor to the recent reduction in bladder cancer mortality, particularly among males. Exposure to some aromatic amines, and particularly 2-naphthylamine and benzidine, is the most important determinant of the excesses of bladder cancer observed in workers from several types of industries. An excess bladder cancer risk was in fact reported more than a century ago among workers employed in dyestuff manufacture, including aromatic amines, whose production has been dramatically reduced since the 1950s. A number of other occupations have been associated with increased risk of bladder cancer, including rubber manufacture, aluminum industry, painting, leather industry, and truck and other drivers, although their risk quantification is mostly undefined. Hair dyes used during the early 1970s contained some mutagenic aromatic amines, and thus occupational use of hair dyes gathered a wide interest and was largely investigated over the last decades in relation to bladder carcinogenesis. In a reanalysis of ten cohort studies including over 81 000 occupationally exposed subjects, it was estimated that there was an overall 40% increased risk of bladder cancer, which was stronger in men (þ60%) than women (þ10%) (La Vecchia and Tavani, 2001). It is unclear whether the risk difference between genders is real or due to other exposures in males (such as to brilliantine) or confounding from smoking or other lifestyle factors. On the other hand, a combined reanalysis of available data excluded any association between personal use of hair dyes and bladder cancer.
Diet
Several substances contained in foods and their metabolites are excreted through the urinary tract, and thus a role of dietary factors in bladder carcinogenesis is plausible.
Consumption of fruit and vegetables, on the one hand, reduced the risk of bladder cancer in a major fraction of studies that investigated the issue. On the other hand, there is some evidence suggesting a direct relation with fat intake. In 2000, Steinmaus et al. conducted a metaanalysis of 38 studies on six dietary variables that gave a relative risk (RR) of 0.7 for high vegetable, 0.8 for high fruit, and 1.4 for high fat intake, whereas no significant association was found for meat (RR = 1.0), retinol (RR = 1.0) or beta-carotene intake (RR = 0.9) (Steinmaus et al., 2000). Recent cohort studies conducted in Eastern Asia found that a high intake of soy was associated with a more than twofold excess bladder cancer risk.
Considering micronutrient intake, results on vitamin A and carotenoids were inconsistent, whereas an inverse association was reported between selenium intake and bladder cancer risk. Long-term use of vitamin E, but not vitamin C, supplements were found to reduce bladder cancer mortality.
With reference to the use of artificial sweeteners, laboratory tests found that large quantities of saccharin cause bladder cancer in rats. In the 1970s, considerable public concern followed the results of an epidemiological study reporting a 60% increased risk of bladder cancer in men (but not women) who used artificial sweeteners (Howe et al., 1977). Nevertheless, large and informative studies conducted thereafter excluded an association with ever use of artificial sweeteners, both in men and women, and according to type or form of sweeteners.
Although it is difficult to separate the effects of single artificial sweetener substances, as these are usually combined in food products, the epidemiologic evidence does not support an association between saccharin and other artificial sweeteners and bladder cancer. Thus, the International Agency for Research on Cancer changed the evaluation of saccharin from group 2B (possibly carcinogenic to humans) to group 3 (not classifiable as to its carcinogenicity to humans).
Fluid Intake
Fluid intake may dilute metabolites in the urine and increase the frequency of voiding, thus reducing contact of carcinogens with the bladder epithelium. According to an opposite theory, the risk of bladder cancer rises with total intake of fluids, as these may contain carcinogenic contaminants too.
Consistently with the first hypothesis, data from the Health Professionals Follow-up Study found that men in the highest fluid intake category had half the risk of bladder cancer as compared to those in the lowest level, and such protection was observed for water as well as for consumption of other fluids (Michaud et al., 1999). However, epidemiological findings on the issue are largely inconsistent, with a majority of case-control studies reporting a direct relation with bladder cancer risk. The issue remains unsettled, due to the extreme difficulties in undertaking and interpreting such studies.
According to the second hypothesis, besides the amount of fluids ingested, the type of beverage and the source of drinking water would be most important. Indeed, a meta-analysis of studies on consumption of chlorinated drinking water found a 40% increased risk for long-term users (Villanueva et al., 2003), and pooled data from six case-control studies gave a higher risk of bladder cancer for consumption of tap water, but no association with non-tap water. High concentrations of arsenic in drinking water, such as those reported in some regions of Taiwan, Bangladesh, Argentina, and Chile, are associated with large increases in risk and incidence of bladder and other cancers, whereas in areas characterized by lower levels of exposure – as the United States and Finland – the pattern of risk is less clear and may be modified by smoking habits.
Beverages
A potential association between coffee drinking and bladder cancer has been investigated since the early 1970s in a large number of epidemiological studies. In 2001, a metaanalysis estimated summary odds ratios (ORs) of 1.26 (95% confidence interval (CI), 1.09–1.46) from studies of male, 1.08 (95% CI, 0.79–1.46) of female, and 1.18 (95% CI, 1.01–1.38) of male and female coffee drinkers combined, after adjustment for smoking (Zeegers et al., 2001). Thereafter, other European cohort and casecontrol studies have reported consistent results that supported these estimates as well as the presence of gender differences in risk. Besides this feature, several studies reported no trend with dose or duration of coffee drinking, and thus coffee is probably not causally related with bladder cancer, although at the same time it may represent an indicator of risk.
Epidemiological findings on a possible relation between alcohol drinking and bladder cancer are compatible with no association or a moderate positive one. The results obtained from various studies are generally inconsistent, and this has been attributed to the fact that various populations have different drinking patterns, as well as different correlates (including coffee and diet) of alcohol drinking. As for coffee consumption, a possible explanation of the moderate increase in risk observed in some studies may be linked to residual confounding by smoking, which is usually directly correlated with both alcohol and coffee consumption, or to an association between alcohol, coffee, and a yet unidentified risk factor.
Urinary Tract And Other Diseases
Bladder cancer is frequent in areas (such as Northern Africa) with a high prevalence of infection with Schistosoma haematobium, which is responsible for chronic irritation of the urothelium. In these areas, a consistent relation between bladder schistosomiasis and cancer has been reported, and the percentage of squamous cell type carcinoma is high (Bedwani et al., 1998).
Chronic irritation of the bladder epithelium caused by urinary tract infections and stones may also increase bladder cancer risk. Various case-control studies reported an approximately twofold excess risk in patients with (recurrent) urinary tract infections, although bladder cancer cases may recall previous urinary diseases more accurately than healthy controls, and thus some of this excess may be explained by recall bias. There is some evidence from both epidemiological and laboratory studies that a history of kidney or urinary stones may moderately increase bladder cancer risk. Microsatellite alterations have been reported in urinary sediments from patients with cystitis and bladder cancer.
Recent prospective and retrospective studies found that subjects with a history of gastric ulcer could share an increased risk of bladder cancer (Michaud et al., 2004). The low antioxidant levels and the bacterial colonization of the stomach occurring during chronic gastritis may explain the association observed, as they lead to endogenous production and subsequent excretion through the urinary bladder of nitrosamines, which are known bladder carcinogens in animals. However, no association emerged with history of duodenal ulcer.
Drugs
The current epidemiological knowledge on the relation between drug use and risk of bladder cancer support an inverse association with non-steroidal anti-inflammatory drugs, a direct association with heavy consumption of phenacetin-containing analgesics (a similar link also emerged with renal cell carcinoma), whereas no consistent relation has been reported for paracetamol. Studies of animal models reported a preventive effect of nonsteroidal anti-inflammatory drugs in bladder carcinogenesis.
Further, there is some evidence that patients treated with cyclophosphamide for non-Hodgkin’s lymphoma had an increased risk of developing bladder cancer, whereas in a few – but not all – studies, treatment with phenobarbital was inversely associated with bladder cancer risk, particularly among smokers.
Family History Of Bladder Cancer
Various retrospective studies consistently reported a 1.5to 2-fold increased risk of bladder cancer in individuals with a history of the same neoplasm in first-degree relatives. These studies were also generally concordant in suggesting that bladder cancer risk is higher when the relatives of bladder cancer patients are diagnosed at early age. Otherwise, a potential involvement of an X-linked susceptibility gene was suggested by findings of higher risks in siblings, and particularly in brothers of young probands, than in offspring of bladder cancer cases, but not all studies found consistent results, and the issue is therefore open to discussion.
There is no evidence in support of an interaction between smoking and familial factors in bladder carcinogenesis, as available data suggest independent effects on risk.
Biomarkers Of Bladder Cancer Susceptibility
Polymorphic distribution of the enzymes involved in the activation and/or deactivation of aromatic amines in humans is an important determinant of individual susceptibility to their carcinogenic effects.
N-acetyltransferase (NAT) is an enzyme whose activity may result in the detoxification of aromatic amines. Its activity in humans is coded by two distinct genes named NAT1 and NAT2. The NAT2 enzyme has long been known to be polymorphic, and in about half of Caucasians, termed slow acetylators, its activity is reduced. Various studies suggested that the slow NAT2 genotype could be a risk factor for bladder cancer, specifically by interacting with occupational exposures to aromatic amines or cigarette smoking, but generally the power to identify significant gene–environment interactions was limited. A first meta-analysis of 22 case-control studies reported an overall RR of bladder cancer for NAT2 slow acetylators of 1.4 (95% CI, 1.2–1.6), as compared to rapid acetylators (Marcus et al., 2000a). Despite significant heterogeneity across studies, this meta-analysis suggested that in most populations slow NAT2 acetylation status is associated with a modest increase in bladder cancer risk. Further, Marcus et al. (2000b) reviewed the relation between cigarette smoking and NAT2 acetylation status in a subsequent meta-analysis of case series that found an interaction between slow acetylation status, tobacco smoking, and bladder cancer risk (RR ¼ 1.3, 95% CI, 1.0–1.6).
There is also a variant polyadenylation signal of the NAT1 gene (NAT1*10 allele) associated with higher enzyme activity (Bell et al., 1995). The activity of NAT1 is reported to be higher than that of NAT2 in the bladder and may increase the formation of DNA binding metabolites of aromatic amines within the target organ. However, less is known about NAT1 polymorphism than about NAT2, and the NAT1 genotype has not been associated with increased risk of bladder cancer.
The enzyme glutathione S-transferase M1 (GSTM1) is involved in the detoxification of a number of carcinogens. About 50% of Caucasians have an inherited deletion of two copies of the gene coding for GSTM1, and several – but not all – studies suggested that individuals homozygous for the deleted genotype (GSTM1 0/0) have an increased risk of bladder cancer. A large Spanish casecontrol study found RRs of 1.2 (95% CI, 0.8–1.7) and 1.9 (95% CI, 1.4–2.7) for individuals with deletion of one or two copies of the GSTM1 gene, respectively (GarciaClosas et al., 2005). The same study also confirmed an increased risk of bladder cancer for NAT2 slow acetylators that was stronger among current smokers.
Most studies do not, however, have adequate power to address the interaction between NAT2, GSTM1, cytochrome P4501A2, environmental factors, and bladder cancer risk. A recent cohort study from Los Angeles provided valuable results highlighting that NAT2 slow acetylators who used permanent hair dyes had a RR of bladder cancer of 2.9 (95% CI 1.2–7.5), and that among lifelong non-smokers, the RR for permanent hair dye use was 6.8 (95% CI 1.7–27.4) for non-NAT1*10 subjects (Gago-Dominguez et al., 2003). Both the estimates were, however, based on few subjects, and much larger studies are required to confirm the associations in subgroups. Therefore, this point is at present unsettled.
Population-Attributable Risks
The population-attributable risk (PAR, i.e., the proportion of bladder cancer attributable to each etiological factor) depends not only on the RR, but also on the frequency of exposure to each factor, and therefore it varies across geographical areas and time periods. The major recognized risk factor for bladder cancer, tobacco smoking, is also the factor to which a large fraction of bladder cancer cases are attributable in most countries, both in men and women. In men, estimates of PAR of bladder cancer related to tobacco smoking varied from 50% in some areas of the United States and in the Netherlands to 70% in Southern Europe and Egypt and to 80% in the UK, whereas in women the PARs were around 30% in developed countries and very low in studies conducted in world areas where tobacco smoking is infrequent in women (such as Egypt). With reference to gene–environment interactions, assuming a RR of bladder cancer of 2.5 for smokers in a predominantly male European population, the PAR was about 35% for slow acetylators who had ever smoked.
It has been estimated that the risk of bladder cancer attributable to occupational factors is between 4 and 7% in Western European countries, and similar results (PARs between 5 and 10%) were previously reported in studies from Great Britain and North America. As the control of occupational exposure to carcinogens improved widely in the last decades in developed countries, the proportion of cases attributable to occupational exposures has probably been declining during recent years. Scanty information is available from other areas of the world, however, where measures to reduce occupational hazard may still be inadequate.
Little information is available on the proportion of cases of bladder cancer attributable to other risk factors, as data are often inadequate to provide useful indications for prevention. Nevertheless, it was estimated that schistosomiasis, a parasitic disease caused by flatworms of the genus Schistosoma, could be responsible of 28% of bladder cancer cases occurring in an urban population of Zimbabwe. Control of schistosomiasis is based on drug treatment, control of freshwater snails that release larval forms of the parasites, improved sanitation, and health education. Thus, reduction of Schistosoma haematobium infection is one of the major preventable causes of bladder neoplasms in various areas of Africa and Middle East. If the association between exposure to chlorination by-products in tap water and bladder cancer is real, the estimated PAR in a Canadian population would be around 15%, while the proportion of bladder cancers attributable to familial and heritable factors was estimated to be relatively low, for example, between 2 and 7%.
In conclusion, there is ample information for prevention and control of bladder cancer. Avoidance of tobacco smoking, close surveillance of occupational exposures to aromatic amines and other chemical agents, and control of bladder and other urinary tract infections would considerably reduce the incidence of bladder cancer worldwide.
Bibliography:
- Bedwani R, Renganathan E, El-Khwsky F, et al. (1998) Schistosomiasis and the risk of bladder cancer in Alexandria, Egypt. British Journal of Cancer 77: 1186–1189.
- Bell DA, Badawi AF, Lang NP, et al. (1995) Polymorphism in the N-acetyltransferase 1 (NAT1) polyadenylation signal: Association of NAT1*10 allele with higher N-acetylation activity in bladder and colon tissue. Cancer Research 55: 5226–5229.
- Bosetti C, Malvezzi M, Chatenoud L, et al. (2005) Trends in cancer mortality in the Americas, 1970–2000. Annals of Oncology 16: 489–511.
- Gago-Dominguez M, Bell DA, Watson MA,, et al. (2003) Permanent hair dyes and bladder cancer: risk modification by cytochrome P4501A2 and N-acetyltransferases 1 and 2. Carcinogenesis 24: 483–489.
- Garcia-Closas M, Malats N, and Silverman D (2005) NAT2 slow acetylation, GSTM1 null genotype, and risk of bladder cancer: results from the Spanish Bladder Cancer Study and meta-analyses. Lancet 366: 649–659.
- Howe GR, Burch JD, Miller AB, et al. (1977) Artificial sweeteners and human bladder cancer. Lancet 2: 578–581.
- International Agency for Research on Cancer (1999) IARC Monographs on the evaluation of the carcinogenic risks to humans, vol. 73. Some chemicals that cause tumours of the kidney or urinary bladder in rodents, and some other substances. Lyon, France: International Agency for Research on Cancer.
- La Vecchia C and Tavani A (2001) Hair dyes and bladder cancer: An update. European Journal of Cancer Prevention 10: 205–208.
- Marcus PM, Vineis P, and Rothman N (2000a) NAT2 slow acetylation and bladder cancer risk: a meta-analysis of 22 case-control studies conducted in the general population. Pharmacogenetics 10: 115–122.
- Marcus PM, Hayes RB, Vineis P, et al. (2000b) Cigarette smoking, N-acetyltransferase 2 acetylation status, and bladder cancer risk: a case-series meta-analysis of a gene-environment interaction. Cancer Epidemiology Biomarkers & Prevention 9: 461–467.
- Michaud DS, Spiegelman D, Clinton SK, et al. (1999) Fluid intake and the risk of bladder cancer in men. New England Journal of Medicine 340: 1390–1397.
- Michaud DS, Mysliwiec PA, Aldoori W, Willett WC, and Giovannucci E (2004) Peptic ulcer disease and the risk of bladder cancer in a prospective study of male health professionals. Cancer Epidemiology Biomarkers & Prevention 13: 250–254.
- Parkin DM, Pisani P, and Ferlay J (1999) Estimates of the worldwide incidence of 25 major cancers in 1990. International Journal of Cancer 80: 827–841.
- Silverman DT, Devesa SS, Moore LE, and Rothman N (2006) Bladder cancer. In: Schottenfeld D and Fraumeni JF Jr (eds.) Cancer Epidemiology and Prevention, 3rd edn., pp. 1101–1127. New York: Oxford University Press.
- Steinmaus CM, Nunez S, and Smith AH (2000) Diet and bladder cancer: a meta-analysis of six dietary variables. American Journal of Epidemiology 151: 693–702.
- Villanueva CM, Fernandez F, Malats N, Grimalt JO, and Kogevinas M (2003) Meta-analysis of studies on individual consumption of chlorinated drinking water and bladder cancer. Journal of Epidemiology & Community Health 57: 166–173.
- Zeegers MP, Tan FE, Goldbohm RA, and van den Brandt PA (2001) Are coffee and tea consumption associated with urinary tract cancer risk? A systematic review and meta-analysis. International Journal of Epidemiology 30: 353–362.
- Brockmo¨ ller J, Kerb R, Drakoulis N, Staffeldt B, and Roots I (1994) Glutathione S-transferase M1 and its variants A and B as host factors of bladder cancer susceptibility: A case-control study. Cancer Research 54: 4103–4111.
- International Agency for Research on Cancer (1987) IARC Monographs on the Evaluation of the Carcinogenic Risks to Humans. Overall Evaluations of Carcinogenicity: An Updating of IARC Monographs Volumes 1 to 42 (Supplement 7). Lyon, France: International Agency for Research on Cancer.
- International Agency for Research on Cancer (2004) IARC Monographs on the Evaluation of the Carcinogenic Risks to Humans, vol. 83. Tobacco Smoke and Involuntary Smoking. Lyon, France: International Agency for Research on Cancer.
- Kogevinas M, ’t Mannetje A, Cordier S, et al. (2003) Occupation and bladder cancer among men in Western Europe. Cancer Causes and Control 14: 907–914.
- Levi F, Lucchini F, Negri E, Boyle P, and La Vecchia C (2004) Cancer mortality in Europe, 1995–1999, and an overview of trends since 1960. International Journal of Cancer 110: 155–169.
- National Research Council, Board on Environmental Studies and Toxicology. Subcommittee to Update the 1999 Arsenic in Drinking Water, Report, Committee on Toxicology (2001) Arsenic in Drinking Water: 2001 update. Washington, DC: National Academy Press.
- Pereg D and Lishner M (2005) Non-steroidal anti-inflammatory drugs for the prevention and treatment of cancer. Journal of Internal Medicine 258: 115–123.
- Van der Meijden AP (1998) Bladder cancer. British Medical Journal 317: 1366–1369.
- Vogelstein B and Kinzler KW (2004) Cancer genes and the pathways they control. Nature Medicine 10: 789–799.
- Zeegers MP, Kellen E, Buntinx F, and van den Brandt PA (2004) The association between smoking, beverage consumption, diet and bladder cancer: a systematic literature review. World Journal of Urology 21: 392–401.
- https://medlineplus.gov/bladdercancer.html – MedlinePlus, U.S. National Library of Medicine and National Institutes of Health: Bladder Cancer.
- https://www.who.int/health-topics/schistosomiasis – World Health Organization: Schistosomiasis.




